Birth of Baby Boy Bau
 |
 |
 |
The arrival of Heidi and David's first child was the happy conclusion to a full night of wakeful labor at the Labor and Delivery Unit at the Hospital of the University of Penssylvania, three long days of contractions, and one "false alarm" stay at the hospital. There were no serious medical complications.
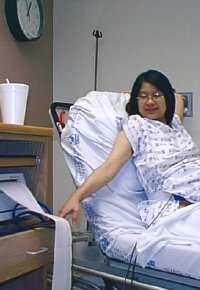
The first stage of labor started Monday night, with contractions so frequent and painful that Heidi was not able to sleep. At Heidi's regular checkup with her gynecologist on Tuesday morning, she was already dialated to three centimeters and having contractions every six minutes: the signs incidated that she was pretty close to delivery. So her doctor sent her upstairs for a stay at the perinatal clinic. In picture two on the right, Heidi is reading the results of the clinic's fetal monitor, which monitors the baby's heartbeat and the mother's contractions. ("Hearing the baby's heartbeat is the best part", Heidi said, "I wish we could take the monitor home.") But it was a false alarm. Several hours passed without much progress, so the family went back home to rest up.
Heidi continued to have contractions all day Tuesday and did not get much rest. But her labor was progressing. By ten at night, her contractions were coming more frequently and regularly, more than 14 each hour. So Heidi, her mother (visiting from Hawaii), and David packed up their hospital kit (packed earlier) and took another trip to the hospital.
On duty last night was a nurse, Michelle, who was Heidi's good friend when they worked together in the Surgical Intenstive Care Unit - Michelle recently transferred to Labor and Delivery. She was assigned to take care of Heidi, and she pampered Heidi through the whole night, bringing everything that was needed: extra blankets, cheerful encouragement, or quick medical help. She stayed past her shift to see through the delivery to the very end.
The couple chose to do the birth under epidural anesthesia. In an epidural block, anesthetic is dripped into the fluid around the spinal cord, numbing pain below a certain point in the body. Unfortunately, Heidi's epidural turned out "one-sided": it was more effective in numbing her right side than her left. Eventually, this meant that the amount of anesthetic needed to numb the pain on her left prevented her from being able to move any muscles on her right. So during the final stage of labor, the anesthetic drip had to be stopped so that she could push effectively. This did not turn out to be a problem.
The other concern was that the doctor found meconium in the amniotic fluid: that is, poop in the womb. The meconium is not a problem by itself, but it makes the baby's first breath dangerous, because if he inhales any dirty fluid, he is in danger of getting serious pnemonia. So at our delivery, the obstretrician used suction as soon as possible to clean out the baby's airways before cutting the umbilical cord, and a pediatric team sat ready to evaluate and treat the baby if any meconium was inhaled - which fortunately, didn't happen. Little David Anthony turned out fine, with no complications.
David Anthony was born articulate and hungry: he cried loudly as soon as his airways were cleared, and continued to cry until he was returned to his mother. And later, he breastfed for more than an hour. (Actually, this soon after birth, babies do not need food, and the mother's breasts do not offer much nutrition; but even if little D.A. was not eating much, he did like to practice.) The next order of the day was a trip to the hospital nursery, where he is sleeping now.
Baby photos will continue to be posted under the "Baby Pics" link in the blue area on the left.





